Aortic Aneurysm/Aortic Dissection
1. What is an Aortic Aneurysm?
2. What is Aortic Dissection?
3. Examination and Diagnostic Methods
4. Treatment Options and St. Luke's International Hospital's Approach
1. What is an Aortic Aneurysm?
✐ Basic explanation and classification of aortic aneurysms
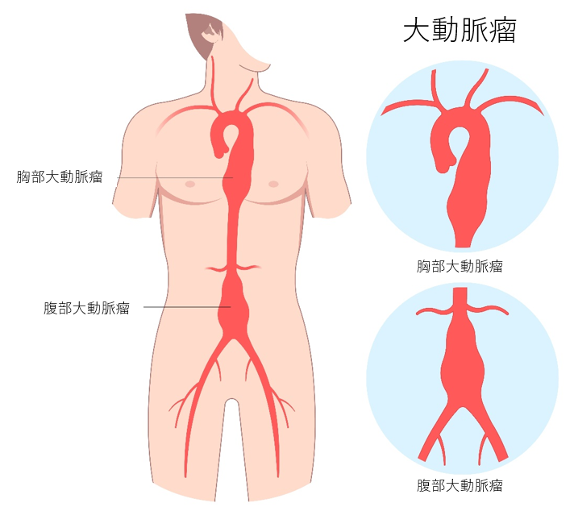
The aorta is the largest artery in the human body, responsible for carrying oxygenated blood from the heart to the rest of the body. After leaving the heart, the aorta ascends through the chest, branches off to supply blood to the head, then descends through the chest and abdomen, branching further before dividing into the legs. The main parts of the aorta are named and broadly classified into the thoracic aorta and abdominal aorta.
An aortic aneurysm refers to a bulging section in the wall of the aorta. It occurs when the aortic wall weakens for some reason and bulges due to blood pressure. Specifically, it can be caused by gradual degeneration of the aortic wall due to aging or atherosclerosis, or by weakening due to trauma, infection, or inflammation. There are also congenital aortic aneurysms that occur in people with conditions like Marfan syndrome or Ehlers-Danlos syndrome, where the arterial walls are inherently fragile and easily stretched. Additionally, aneurysms that develop secondarily in a weakened aorta due to aortic dissection (discussed later) are specifically called dissecting aortic aneurysms.
Among these causes, traumatic, infectious, inflammatory, and congenital factors can occur at any age, so even relatively young people can develop aortic aneurysms. Special caution is needed if you have a family member diagnosed with an aortic aneurysm.
So, at what size is it called an aortic aneurysm?
The normal size of the aorta varies by location. While there are individual differences, generally, it’s considered 30mm in the chest and 20mm in the abdomen. An aortic aneurysm is defined when the expansion exceeds 1.5 times the normal size. Therefore, 45mm or more in the chest and 30mm or more in the abdomen are diagnosed as thoracic aortic aneurysm and abdominal aortic aneurysm respectively.
Based on their shape, aneurysms that bulge all around are classified as fusiform aneurysms, while those that bulge partially outward are classified as saccular aneurysms. These classifications are extremely important as the risk of rupture differs depending on the shape.
✐ Symptoms and risk factors of aortic aneurysms
Aortic aneurysms are usually asymptomatic in the early stages, making them difficult to detect.
As the aneurysm expands, compression symptoms may appear due to pressure on surrounding organs. If an aortic aneurysm is discovered late, it can eventually rupture inside the body, causing sudden severe pain in the chest, abdomen, or back, and symptoms associated with bleeding (low blood pressure, difficulty breathing, altered consciousness, hemoptysis or hematemesis), leading to a critical condition with a high risk of death.
If you have any of the following symptoms, there’s a possibility of an aortic aneurysm, and we recommend getting a medical examination:
Symptoms:
• Discomfort or pressure in the chest or abdomen (difficulty breathing, abdominal bloating)
• Hoarseness or being told your voice has changed (dysphonia; symptom of pressure on the vocal cord nerves)
• Difficulty swallowing or feeling of something stuck in the throat (dysphagia; symptom of esophageal compression)
• Loss of appetite, feeling full quickly, nausea after eating (symptoms of gastrointestinal compression)
• Feeling a pulsating mass in the abdomen
Risk factors for aortic aneurysms vary by individual, but common factors include:
• Hypertension
• Smoking
• Dyslipidemia (high cholesterol)
• Genetic factors (family history of aortic aneurysm or aortic dissection)
• Aging
• Obesity
Controlling risk factors is important not only for preventing the onset of aortic aneurysms but also for preventing rupture. However, it’s not a guarantee that you won’t develop an aortic aneurysm or that an existing aneurysm will heal just by being careful. Early diagnosis and treatment at a medical institution are particularly important for those at high risk. At St. Luke’s International Hospital, we provide thorough follow-up care, including control of risk factors.
2. What is Aortic Dissection?
✐ Basic explanation and classification of aortic dissection
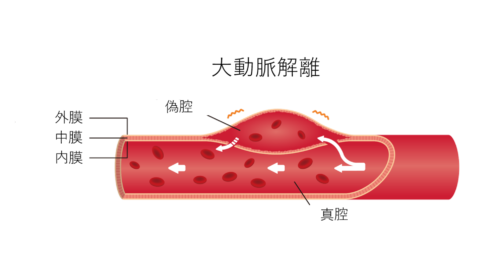
The aorta has a three-layer structure, consisting of the intima, media, and adventitia from the inside out. Acute aortic dissection is an acute-onset condition where a tear occurs in the intima for some reason, causing it to separate from the media. When dissection occurs, blood can enter between the layers of the aortic wall, creating what appears to be two blood flow pathways. The normal blood flow path inside the intima is called the true lumen, while the space created between the intima and media is called the false lumen.
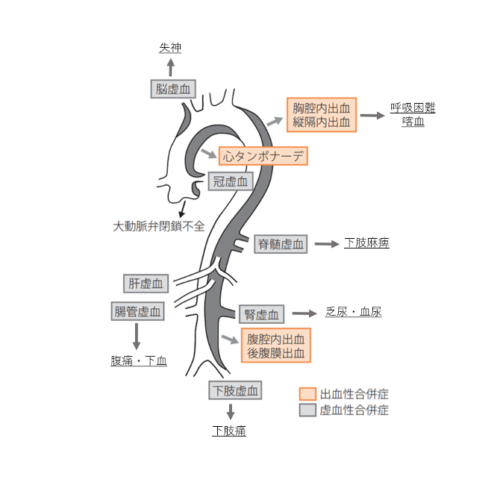
The part of the aorta where dissection has occurred becomes thin and fragile, risking rupture and massive internal bleeding. Additionally, the false lumen can impede blood flow to various organs, potentially causing symptoms of organ ischemia (branch perfusion disorder or malperfusion) such as stroke, renal ischemia, and lower limb ischemia. If the dissection spreads close to the heart, it can even cause symptoms like myocardial infarction or aortic valve regurgitation, making it an extremely high-risk emergency condition that can be life-threatening.
While the exact cause of aortic dissection is still not fully understood, it’s thought that sustained high pressure on the aortic wall, such as from hypertension, weakens the media over time, and then the intima tears during some physical activity. Like aortic aneurysms, congenital conditions that cause inherent tissue fragility, such as Marfan syndrome or Ehlers-Danlos syndrome, are also causes of aortic dissection. Special caution is needed if you have a family member who has experienced aortic dissection.
Additionally, aortic dissection can also be caused by trauma such as traffic accidents or injuries, which is another important life-threatening cause.
There are various classifications of aortic dissection, but the Stanford classification, which is based on location, is particularly important as it relates to treatment strategies.
Stanford Type A: Aortic dissection that involves the ascending aorta close to the heart
Stanford Type B: Aortic dissection that does not involve the ascending aorta close to the heart
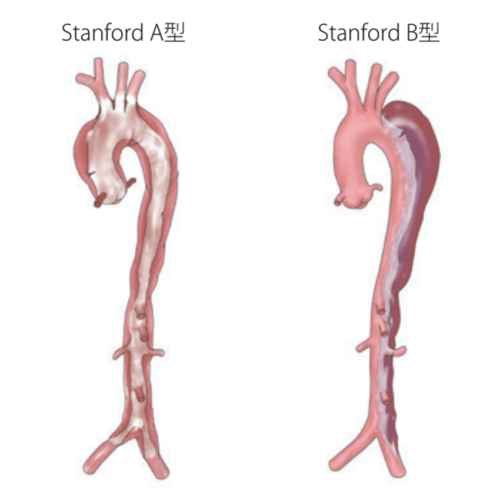
Generally, Stanford Type A, which involves the ascending aorta (close to the heart and branching to supply blood to the brain), is considered more dangerous and potentially fatal. However, Stanford Type B can also pose life-threatening serious complications, and a more detailed assessment of the aortic dissection condition and prompt determination of treatment strategy require management by an experienced heart team.
✐ Symptoms and risk factors of aortic dissection
Aortic dissection is often acute in onset and accompanied by severe symptoms. Specifically, chest, back, or abdominal pain that is described as “unlike anything experienced before,” “like being cut with a knife,” or “moving from one location to another” is characteristic. However, diagnosis can be difficult in many cases as it may be indistinguishable from other conditions due to individual variations in pain intensity and location depending on the site and onset form of the dissection. Sometimes, the progression of dissection may temporarily stop, causing the pain to subside, which can lead to dangerous situations where patients don’t seek medical attention.
Furthermore, if ischemic symptoms in various organs occur due to the aforementioned branch perfusion disorder, it can present with diverse symptoms such as syncope, weakness in the upper or lower limbs, abdominal pain and bloody stools, hematuria, or difficulty breathing. This further complicates the diagnosis of aortic dissection.
Risk factors are similar to those for aortic aneurysms and include:
• Hypertension
• Smoking
• Dyslipidemia
• Genetic factors (family history of aortic aneurysm or aortic dissection)
• Aging
• Obesity
• Physical and mental stress
Additionally, about half of Stanford Type A aortic dissections are known to be associated with sleep disorders. Besides insomnia and sleep deprivation, sleep apnea syndrome is strongly associated with aortic dissection and subsequent progression to dissecting aortic aneurysm. If you experience symptoms such as “stopping breathing during sleep” or “family members point out your snoring,” we strongly recommend early medical consultation.
3. Examination and Diagnostic Methods
✐ Diagnostic methods for aortic aneurysm and aortic dissection
Diagnosing aortic aneurysms and aortic dissections requires specialized examinations and diagnostic methods. Imaging diagnosis is particularly important, and various examination methods exist. It’s important to note that while unruptured aortic aneurysms are often discovered during health check-ups, human dock examinations, or incidentally during consultations for other conditions, ruptured aortic aneurysms/acute aortic dissections are typically diagnosed during emergency consultations. Therefore, the choice of examination may vary depending on the presence or absence of symptoms.
The following are the main methods used to diagnose these conditions:
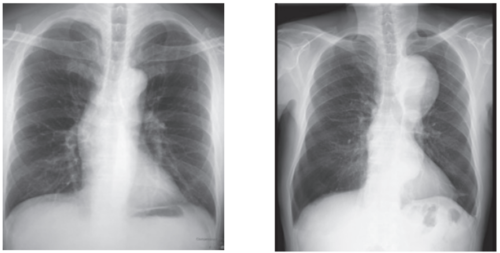
• Plain X-ray
This is generally referred to as a chest X-ray or abdominal X-ray. Plain X-rays are used for initial screening to evaluate the shape and degree of enlargement of the aorta. These are often taken during health check-ups and frequently lead to referrals for more detailed examinations.
However, it’s important to note that aortic aneurysms and aortic dissectionsmay not be recognizable on plain X-rays unless the aorta is significantly enlarged or there is severe arteriosclerosis or calcification.
• Ultrasound examination (Echo examination)
This includes items called echocardiography and abdominal ultrasound, which may be optional in health check-ups or human dock examinations. It’s a screening tool for evaluating the shape and degree of enlargement of the aorta, with the advantage of being less burdensome (non-invasive) for patients. It can relatively accurately assess the size of the aorta and can even visualize the shape of aortic aneurysms and the internal structure of aortic dissections. Similar to plain X-rays, many cases lead to consultations for detailed examinations based on ultrasound results.
Additionally, it allows for rapid and real-time evaluation of the aorta in emergency situations. At our hospital, we actively perform bedside ultrasound examinations by emergency department, cardiovascular surgery, and cardiology physicians immediately upon arrival to pursue rapid diagnosis..
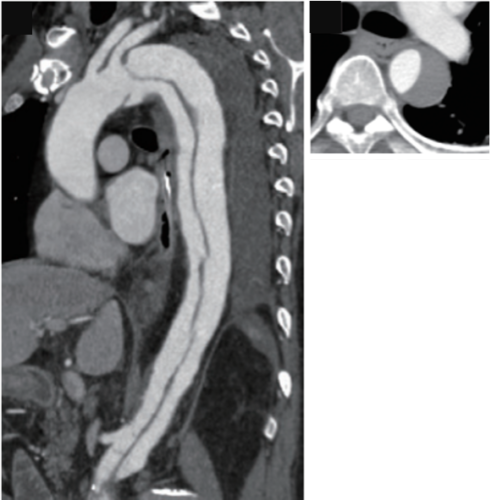
• CT scan (Computed Tomography)
CT scans provide detailed internal information from cross-sectional images of the body and are necessary precision examinations for the definitive diagnosis of aortic aneurysms and aortic dissections. Contrast-enhanced CT, which involves injecting contrast agent into the body through an IV during imaging, is used to obtain a more accurate view of the aortic shape. However, in some cases, a diagnosis can be made with non-contrast CT alone. In addition to revealing organ ischemia symptoms caused by aortic dissection, this examination is essential for developing treatment plans for aortic aneurysms and dissections. It is also regularly performed in outpatient settings to monitor aortic aneurysms that don’t require immediate treatment but need follow-up, as well as for post-operative progress checks.
· MRI (Magnetic Resonance Imaging)
For patients who cannot use contrast agents due to allergies or severe kidney dysfunction,At St. Luke’s International Hospital, alternative imaging examinations without using contrast agents are possible with MRI.While MRI takes longer to perform compared to contrast-enhanced CT, it is known to have a comparable diagnostic rate to CT. It is a useful examination as there is no X-ray exposure or use of contrast agents. It can also evaluate the presence of inflammation and is superior for qualitative diagnosis to identify causes. Although not suitable for emergencies such as aortic aneurysm rupture or acute aortic dissection, it is appropriate for follow-up and preoperative examinations.
If you have the above symptoms or risk factors and are concerned about aortic diseases, please undergo a thorough examination with the above tests and feel free to consult our Cardiovascular Center at any time.
4. Treatment Options and Our Hospital’s Approach
At St. Luke’s International Hospital’s Cardiovascular Center, an experienced heart team consisting of cardiovascular surgery, cardiology, anesthesiology, nurses, clinical engineers, and cardiac rehabilitation instructors provides cutting-edge aortic disease treatment with the motto ‘Safely, the best treatment’.
We will explain the treatments for aortic aneurysm and aortic dissection, along with introducing our hospital’s approach.
✐Treatment for Aortic Aneurysm/Aortic Dissection
・Drug Treatment
While there is no direct drug treatment for aortic aneurysms, in the early stages of aortic aneurysm or for small aneurysms before surgical indication, medications for risk factors such as hypertension may be prescribed. Generally, antihypertensive drugs are used to stabilize blood pressure and reduce the burden on the aorta. Drug therapy is expected to suppress the growth of the aneurysm.
In addition, treatments for lipid control, smoking cessation, and sleep apnea syndrome are very important for managing risk factors.
The treatment method for aortic dissection differs between Stanford Type A and Type B. In Type A cases, the mortality rate is extremely high without surgical treatment, so emergency surgery is chosen except for special types. For Type B,
・No signs of rupture
・No symptoms of organ ischemia
・Stable condition without persistent pain or high blood pressure
Under these conditions, conservative treatment with drug therapy alone may be chosen.
In this case, the treatment aims to stabilize the dissected aorta by maintaining rest under strict blood pressure and heart rate management with intravenous medications in the intensive care unit.
・Surgical Treatment via Thoracotomy or Laparotomy
Surgical Treatment for Aortic Aneurysm:
Surgery may be necessary when an aortic aneurysm grows rapidly, has a high risk of rupture, or expands beyond a certain size. It is important to carefully evaluate and determine surgical indications based on the location and shape of the aortic aneurysm, rate of expansion, age, body type, and coexisting conditions. Emergency surgery is performed in cases of aortic aneurysm rupture or acute aortic dissection Stanford Type A.
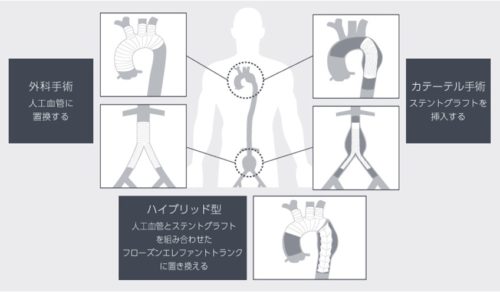
Surgery is performed through thoracotomy or laparotomy. The affected portion of the aorta is removed and replaced with an artificial graft. This is called artificial graft replacement. The surgical technique varies depending on the location, as shown in the figure below.
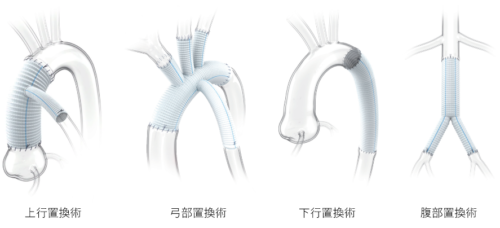
Artificial grafts are specialized tubular devices used to replace the function of normal blood vessels. These vessels play a role in effectively transporting blood within the body. Modern artificial grafts, mainly made of materials such as polyester, can function for long periods, are safe to use, have excellent biocompatibility and antithrombogenicity, and if there are no problems after surgery, they can be implanted semi-permanently, and blood-thinning medications are generally not necessary.
Artificial graft replacement requires temporarily blocking blood flow to the aorta, and depending on the location, there may be a period called ‘circulatory arrest’ where blood flow to the entire body, including the heart, is stopped. Therefore, advanced cardiopulmonary bypass techniques are required to cool the patient’s body to extremely low temperatures or to send blood flow only to vital organs such as the brain to prevent complications like stroke. Although the physical burden = invasiveness on the patient is significant, it is also the most reliable treatment in terms of certainty of treatment, which cannot be replaced by alternatives.
・Endovascular Treatment
For some cases of enlarged aortic aneurysms, endovascular treatment called stent graft insertion can be an alternative to surgery performed through thoracotomy or laparotomy. This involves inserting an artificial blood vessel (graft) with an integrated metal skeleton (stent) through the femoral artery in the groin and deploying it within the aorta to isolate the aortic aneurysm wall from blood flow pressure.
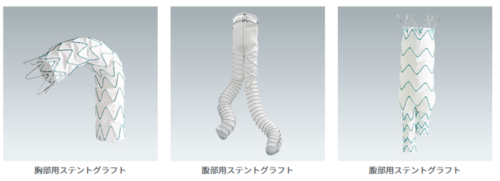
There are various models currently available in Japan, expanding treatment options. Like artificial grafts, these stent grafts can be implanted semi-permanently if no problems occur.
Endovascular treatment has the advantage of being minimally invasive, with smaller incisions, shorter operation times, and faster postoperative recovery for patients. However, it should be noted that long-term results are still not as good as artificial graft replacement, and it may not be applicable due to individual anatomical differences such as severe aortic tortuosity or calcification.
Stent graft insertion can also be used in some emergency cases such as aortic aneurysm rupture or acute aortic dissection, and is gaining attention as a treatment that increases survival rates with minimal invasiveness.
✐ Our Hospital’s Approach to Aortic Disease Treatment
The Cardiovascular Center at St. Luke’s International Hospital performed 65 cases of aortic disease surgeries in 2022. Additionally, we are part of the ‘Acute Aortic Super Network’, an emergency care system for acute aortic diseases in Tokyo, and are certified as an emergency aortic support hospital capable of prioritizing admission and surgery for acute aortic diseases.
Our heart team not only focuses on early diagnosis and treatment but also proposes and provides treatment plans tailored to each individual patient.
At our hospital, for lesions extending over a wide range of the aorta or cases with complex anatomy, we also perform two-stage hybrid treatment combining artificial graft replacement and stent graft insertion. Additionally, for patients who normally cannot undergo stent graft insertion due to the risk of occluding branch arteries, we can make stent graft insertion possible by simultaneously performing branch artery bypass reconstruction.
A recent initiative in stent graft insertion at our hospital is the introduction of ‘Percutaneous Stent Graft Insertion’, which can be completed with a minimal incision of less than 1 cm without any cutting or suturing, further refining our minimally invasive approach. For scheduled surgeries, patients can be discharged in about 2-3 days after the procedure. Furthermore, our hospital’s strength lies in handling special cases that require specialized internal medicine treatment, such as infected aortic aneurysms.
These aortic diseases require drug treatment and careful follow-up from early diagnosis, in cooperation with primary care physicians. St. Luke’s International Hospital’s Cardiovascular Center emphasizes regional collaboration and actively engages in continuing internal medicine treatment, not just surgical treatment, to comprehensively protect patients’ health.
If you have concerns about aortic disease treatment, please don’t hesitate to consult with us.