Cardiac Catheterization (Coronary Angiography) Procedure at Our Hospital
For patients scheduled for cardiac catheterization (coronary angiography) at our hospital, we have summarized a brief overview of the examination and treatment process.
Please note that the content introduced here is specific to our hospital, so there may be differences in examinations and treatments at other hospitals.
Also, please understand that even at our hospital, the process may differ from what is described here depending on the patient’s condition and circumstances.
※ Some videos are included, but none contain audio.
1 To the Catheterization Room
1.1 Hospital Room
All rooms in our hospital are private and equipped with a toilet, TV, and washbasin. For inpatient catheterization examinations and treatments, you can relax here before and after the procedure.


1.2 Catheterization Examination Gown
For catheterization examination and treatment, you will change into a special gown in your hospital room. You will also be asked to wear a mask and cap before entering the room (we will provide these).

1.3 Transfer
You will be moved from your hospital room to the catheterization room by walking, wheelchair, or transfer bed. The catheterization room is located on the 5th floor of our main building.
1.4 Patient Identification Before the Catheterization Room
Before entering the catheterization room, you will be asked to state your full name and date of birth for identification purposes.

1.5 If Family Members Accompany
Accompanying family members or related persons will be asked to wait in the waiting area (open space) in the 5th floor lobby. There are toilets and vending machines nearby for your use if needed.

2 Examination Preparation
2.1 About the Catheterization Room
Our hospital has two catheterization rooms. There are no significant differences in performance or specifications, but the attending physician will decide which examination room to use based on the patient’s condition and availability.
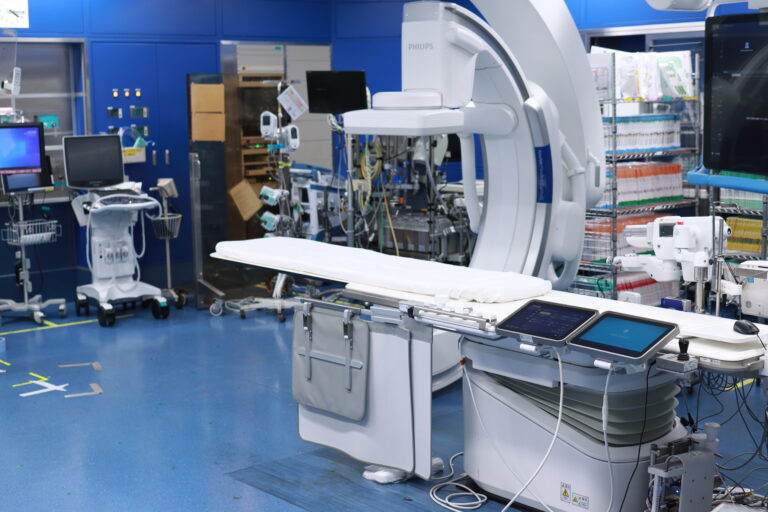
2.2 Catheterization Table
The catheterization table is slightly narrow in width. This is because the radiation equipment moves to observe the heart from various angles. Even for larger individuals, there is no danger as long as you don’t move significantly, but as mentioned later (refer to ‘3.6 Notes on Maintaining Posture’), please try not to move during the examination and treatment. If you have any requests, please verbally inform the staff.
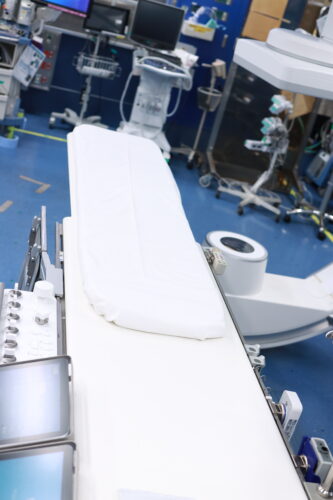
2.3 Moving to the Catheterization Table
Following the nurse’s guidance, you will sit on the catheterization table and then lie down on your back. We will support you to ensure there is no danger.
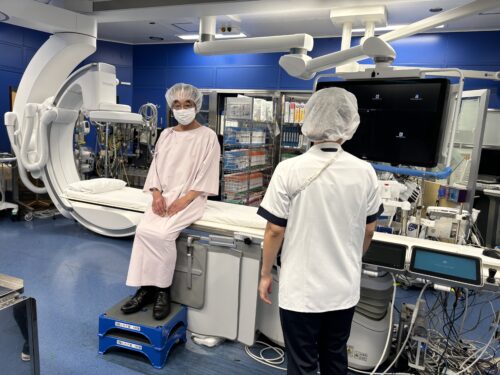
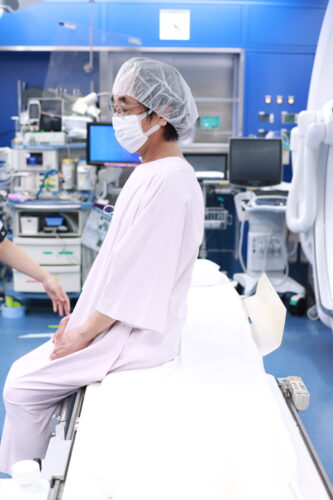
2.4 Monitor Preparation
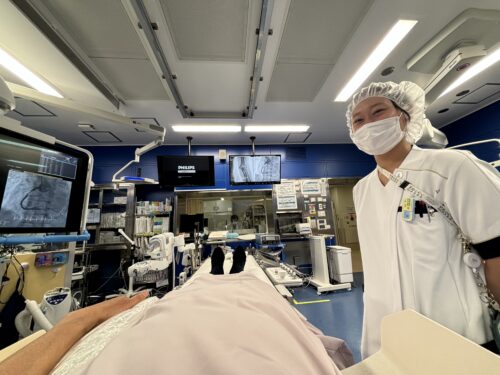
This is an image from the patient’s perspective. In this state, we will attach monitors such as ECG and oxygen saturation meter, and secure or check the IV line as preliminary preparation. As there is a possibility of feeling the urge to urinate due to the use of contrast media, we may provide a urinal or diaper if there is a possibility of treatment or if the examination may be prolonged.
2.5 Confirmation of Puncture Site
At our hospital, we typically perform catheterization through the left radial artery, which is the artery in the wrist (the blood vessel you often feel when checking your pulse). For patients undergoing hemodialysis, those with arteries too thin for puncture, or cases where catheterization from a larger blood vessel is preferable, we may perform catheterization from other blood vessels such as the elbow or groin.
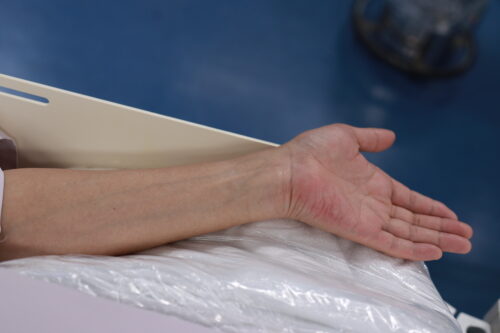
As mentioned later (refer to ‘Our Hospital’s Measures to Address ‘Pain’ During Examination and Treatment’), to minimize pain during the examination, we apply an anesthetic tape called Penles Tape to the puncture site for patients who are already admitted. The Penles Tape is removed during this puncture site confirmation.
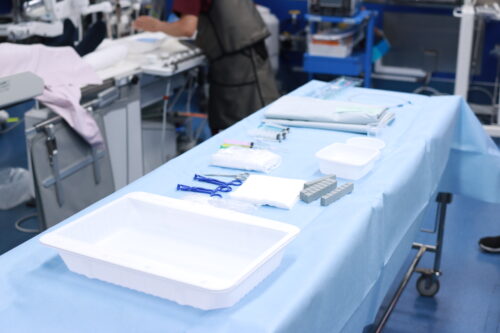
This is a sterile table for placing instruments and medications used in the examination. The necessary instruments for the examination and treatment are prepared in advance in a sterile condition for use.
3 Before Starting the Examination
3.1 Disinfection, Draping
We will disinfect the puncture site. Basically, we use alcohol disinfection which has a strong sterilizing effect, but for those with alcohol allergies, we use iodine disinfection. In cases where treatment is possible, even if the examination and treatment are planned from the wrist, we will also disinfect the groin area as a precaution for unforeseen circumstances, so please understand.
After disinfection, we cover areas other than the puncture site with a sterile cover (drape).
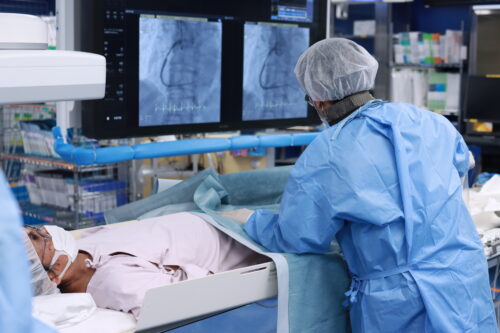
3.2 Time Out
Just before administering local anesthesia, we perform a final patient identification and joint confirmation among staff that the examination preparation has been completed without any issues. The nurse will ask you to cooperate in confirming your name (full name) and date of birth.
3.3 Local Anesthesia, Puncture
First, we inject local anesthetic into the subcutaneous tissue at the puncture site using an extremely fine needle. We will perform the main puncture after confirming that the pain has been sufficiently reduced.
◎ Our Hospital’s Measures to Address ‘Pain’ During Examination and Treatment
At our hospital, we
focus on minimizing patient pain caused by the procedure
.
At our hospital, whenever possible, we perform catheter examinations and treatments from the wrist, which is considered the least invasive (in some cases, we may have to choose examination and treatment from other sites depending on the thickness of blood vessels or the complexity of treatment). Before moving to the catheterization room, we apply anesthetic tape (Penles Tape) to the planned puncture site to reduce pain, and before the main puncture, we administer local anesthesia with a sufficient amount of anesthetic using an extremely fine needle. Also, regarding the size of the catheter to be inserted, we basically use a small-diameter sheath called a glide sheath (please refer to this) to minimize the invasiveness to blood vessels during the examination.
During treatment, you may experience chest discomfort while a balloon is being used to expand the stenotic area or while a stent is being placed. If you experience severe pain or discomfort, please don’t hesitate to speak up, as we may consider administering pain relief injections depending on the situation.
3.4 Sheath Insertion
Once a wire has been passed into the blood vessel through the puncture, we first insert a tube called a sheath that connects the inside of the blood vessel to the outside world. The sheath has a hemostasis valve, which prevents bleeding from there or air from entering. We will perform the examination and treatment by inserting and removing catheters through this sheath.

3.5 Heparin Administration
We administer heparin, a blood-thinning medication, through the sheath. You may feel the area where the sheath is inserted become hot or cold, but this is only temporary and not a problem.
This completes the preparation for inserting the catheter. You should not feel much pain during the catheter examination, but if you do experience severe pain, please don’t hesitate to speak up.
3.6 Notes on Maintaining Posture
During catheter examination and treatment, you can communicate with staff or express yourself, but you basically cannot move your body. This is because the catheter table is very narrow due to the movement of the radiation equipment, and there is a risk of falling if you move significantly. Additionally, moving the area where the catheter is inserted can be very dangerous as it may damage the heart or blood vessels with the catheter. Therefore, even if your nose itches, your hat or mask slips, your back hurts, your feet feel numb, or you feel cold, never move on your own and always inform the staff first. You can sleep or cough during the examination (we will notify you if you need to be awake for examination or treatment purposes).
4 During the Examination
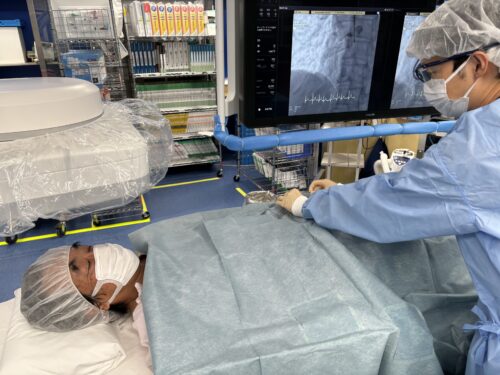
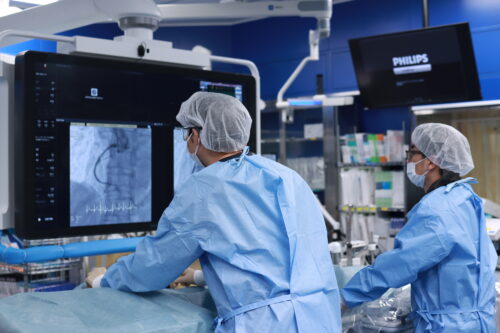
4.1 Operator
In the case of the approach from the left wrist, which is commonly performed at our hospital, the operator straddles the body to manipulate the catheter, as shown in the photo.
The examination and treatment are basically performed by two or more doctors, with the first operator manipulating the catheter and the second operator operating the catheter table and radiation equipment.
4.2 Types of Catheters
Different shapes of catheters are used according to the shape of the coronary arteries and aorta. The most commonly used are the Judkins Left for the left coronary artery and the Judkins Right for the right coronary artery.
4.3 Precautions for Contrast Agent
During the examination, contrast agent is injected into the bloodstream through the catheter. While contrast agent is essential for catheter examination, it is also known to be prone to causing allergies. If you experience itching, respiratory symptoms, or nausea during the examination, please inform the staff immediately.
4.4 Movement of Radiation Tube, Table Up and Down
When injecting contrast agent into the coronary arteries, we observe the coronary arteries from various angles to avoid missing any stenosis or occlusion. At this time, the radiation equipment moves, and the table moves up, down, left, and right. Although there are safety mechanisms and there is basically no danger to the patient from the machine’s movement, the sterile cover bags attached to the equipment may occasionally touch your face or body. If this is uncomfortable, please inform the staff.
4.5 Ischemia Function Evaluation
When coronary angiography reveals actual narrowing of the coronary arteries, we may proceed with an ischemia function evaluation using a special wire.
If the blood flow reduction due to stenotic lesions is severe, the need for treatment to improve blood flow increases. However, it has been found that the body’s mechanism for regulating cardiac blood flow is complex, and it is difficult to judge this solely by the ‘appearance (stenosis rate)’ on images obtained from catheter examination. For example, even if two lesions have the same stenosis rate of 50%, the severity of blood flow reduction due to stenosis may differ depending on the length of the lesion and the amount of myocardium downstream. Therefore, it is considered appropriate to decide whether to place a stent in a narrowed coronary artery lesion based on the ‘rate of blood flow reduction’ rather than the ‘appearance’. The examination to measure this blood flow is called FFR (Fractional Flow Reserve) examination, which can measure how much blood flow is reduced before and after the lesion by inserting a special wire into the coronary artery and measuring the pressure inside the vessel before and after the narrowed lesion.
Recently, as an alternative to the conventional wire-based blood flow measurement, coronary blood flow analysis software has been developed. A representative example is the quantitative flow ratio (QFR) software, which is also implemented in our hospital. For more details, please see here.
4.6 Patient’s Perspective Images and Videos During Examination

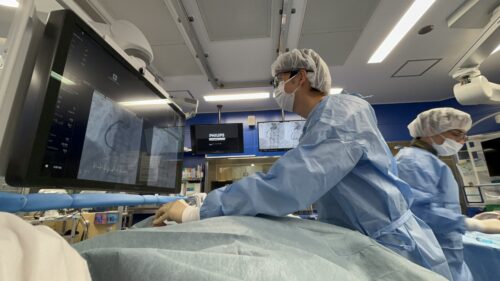
These are images and videos from the patient’s perspective during the examination. Depending on the angle, you may be able to see the screen displaying the examination footage, but please refrain from trying to sit up to see it better.
4.7 Additional Examinations
If no coronary artery stenosis requiring treatment is found during the coronary angiography, the examination may end, or additional tests may be performed. If there is a possibility of needing additional tests, we explain this possibility at the time of providing the consent form.
If coronary vasospastic angina is suspected, we may perform a coronary spasm provocation test. If coronary microvascular dysfunction is suspected, we may perform a coronary microvascular resistance measurement test.
5 Treatment
If the results of the coronary angiography indicate that catheter treatment is necessary, we will either schedule the treatment for a later date or proceed from examination to treatment immediately. If there is a possibility of proceeding to treatment directly after the examination, we explain this possibility and obtain consent for the treatment when providing the examination explanation and consent form in advance. Please note that same-day catheter treatment is not possible for outpatient catheter examinations. Also, even if treatment is planned after the examination, depending on the results of the catheter examination, we may reschedule the treatment for a different date or determine that surgical intervention is necessary instead of catheter treatment.
When transitioning from examination to treatment, we will replace the catheter and administer additional blood-thinning medication. Other precautions are mostly the same as for the catheter examination, but you may experience discomfort in your chest when the balloon is inflated or when the stent is being placed. If you experience any chest symptoms, please inform the staff verbally without moving your body.
For more details about catheter treatment, please see here.
6 End of Examination/Treatment
6.1 Hemostasis Technique (TR Band)
When the examination or treatment is completed and the sheath is removed, hemostasis is necessary. Unlike venous hemostasis, arterial hemostasis requires compression for several hours.
If the examination or treatment was performed from the wrist, we use a special band as shown in the photo below for hemostasis. It’s called a TR Band, which inflates a rubber balloon inside the band by injecting air, compressing the puncture site for hemostasis.
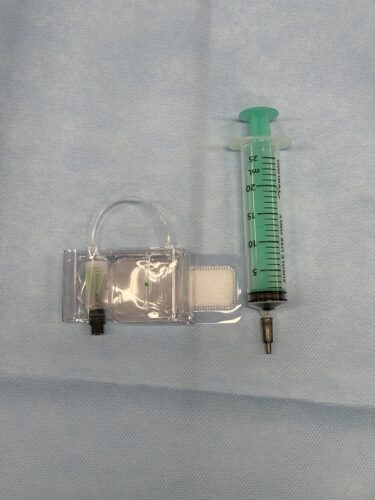
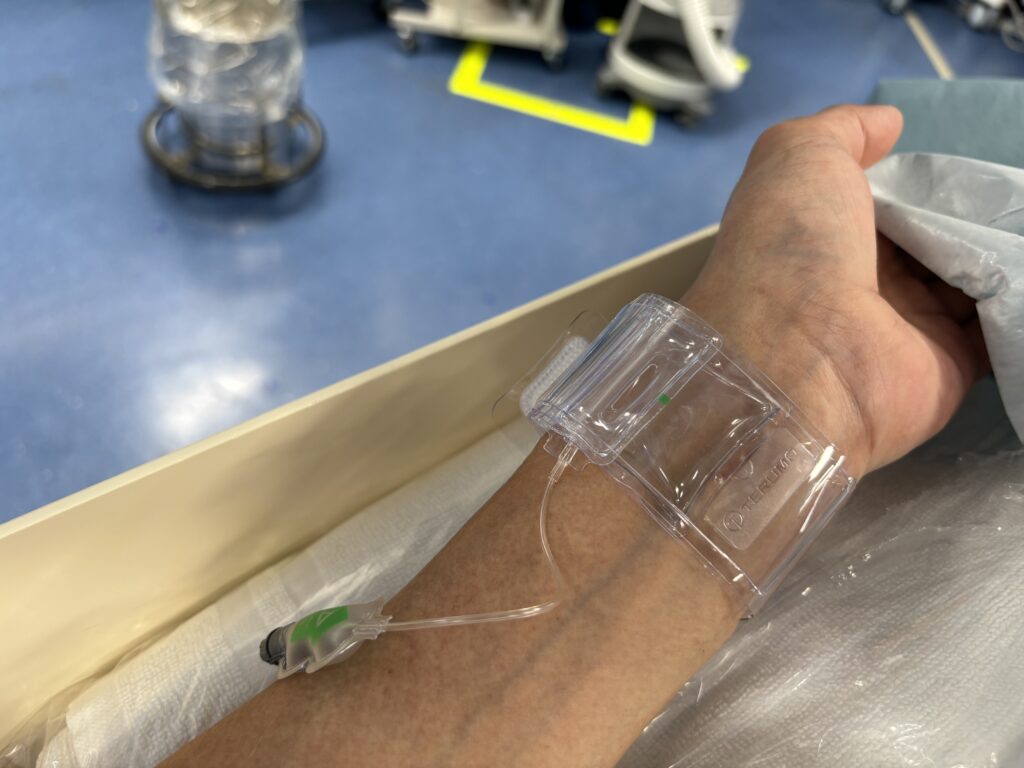
6.2 Sign-out
Finally, all staff members confirm and share information about what examination or treatment was performed, what results were obtained, the patient’s current condition, post-procedure precautions, and whether there are any samples to be submitted, before concluding the procedure.
6.3 Explanation of Results
The results of the catheter examination or treatment will be explained directly by the attending physician. A brief verbal explanation will be given at the end of the examination or treatment, and later, we will visit your room to provide a more detailed explanation and discuss future plans.
If your family members are waiting in the waiting room, we may provide them with a verbal explanation of the results first.
6.4 Returning to the Room
Once the monitoring equipment is removed and preparations for leaving the catheter room are complete, you will return to your original room. If you are hospitalized, you will return to your hospital room, and if it’s an outpatient catheter examination, you will return to the waiting room on the 5th floor. If you are hospitalized and your family members are waiting in the waiting room on the 5th floor, the nurse will call them when you are moving, so they can return to the room with you.
The method of movement is generally the same as when entering the catheter room, but if the catheter was inserted from the groin area or if sedatives were used during the examination or treatment, you will be moved using a bed.
7 Post-Procedure Precautions and Discharge
7.1 Different Precautions Based on Puncture Site
If the examination was performed from the wrist, you will generally wear the band for about 4-5 hours. If the examination was performed from the elbow or leg (refer to ‘2.5 Confirmation of Puncture Site’), the attending physician will determine based on the location and hemostasis method. Especially if the examination or treatment was performed from the groin area, you will need to rest in bed for a while (at least 3 hours or more). If the examination or treatment was from the wrist, it’s okay to walk, but avoid excessive bending of the punctured wrist or applying strong force.
7.2 If Bleeding Occurs or Swelling Appears at the Puncture Site
Use the nurse call immediately to summon staff. You may press on the bleeding area over the band or compression device, but never remove the band or compression device yourself.
7.3 For Outpatient Catheter Examinations
Generally, the examination starts at 9:15 AM and takes about 30 minutes to 1 hour. Before and after the examination, you will rest in a dedicated rest area on the 5th floor. Typically, the TR Band is removed around 3 PM, and you can go home. However, if hemostasis takes longer, you may need to stay until the evening.
7.4 For Same-Day Admission
Similar to outpatient examinations, the examination is performed in the morning, and you may be able to discharge after 3 PM. You will spend time before and after the examination in a hospital room.
7.5 Estimated Discharge Time for Next-Day Discharge and Precautions
For typical inpatient catheter examinations or treatments, if there are no issues confirmed in the morning of the following day, discharge is usually scheduled for around 10 AM.
7.6 Precautions After Returning Home
On the day of the catheter examination, you can take a bath, but only lightly rinse the area where the catheter was inserted without submerging it in the bathtub. From the next day onwards, you can soak in the bathtub. However, if you receive specific instructions from the attending staff, please prioritize those instructions.
If you experience bleeding or swelling at the puncture site after returning home, please contact our hospital (03-3541-5151).