Ischemic Heart Disease – About Treatment
Our center is prepared to respond immediately to patients requiring emergency treatment, no matter how severe their condition, at any time. For patients who have sufficient time before treatment, we propose the optimal treatment for each individual patient.
- Treatment for Acute Myocardial Infarction (Acute Coronary Syndrome)
- Treatment for Angina Pectoris (Chronic Coronary Syndrome)
- Percutaneous Coronary Intervention (Catheter Treatment)
- Coronary Artery Bypass Surgery
- Shockwave (IVL) for Safe Treatment of Heavily Calcified Lesions
- Comprehensive Medical Care by the Heart Team
- Safe and Short Hospital Stays
Treatment for Acute Myocardial Infarction (Acute Coronary Syndrome)
To provide treatment as quickly as possible, we are prepared to treat even the most critically ill patients 24 hours a day, 365 days a year, in collaboration with our hospital’s emergency center
Acute myocardial infarction, where a coronary artery is suddenly blocked by a blood clot, can be life-threatening and often requires immediate attention. For the most urgent form of acute myocardial infarction (ST-elevation myocardial infarction), it is known that restoring blood flow as quickly as possible through catheter treatment using balloons or stents improves patient prognosis (survival rate). Our hospital maintains a system where cardiologists capable of performing catheter treatments are available 24 hours a day, 365 days a year, aiming to restore blood flow through catheter treatment within 90 minutes of arrival. Additionally, for patients with issues in multiple coronary arteries, bypass surgery may be the appropriate treatment choice, and in such cases, we also have a system in place where cardiovascular surgeons can perform surgery without delay at any time. Furthermore, our hospital strives to provide treatment at any time for any patient in an emergency, not just for our regular patients.
As our hospital is a tertiary emergency designated hospital with an emergency and critical care center capable of accepting the most critically ill patients, we are equipped with extracorporeal membrane oxygenation (ECMO) and IMPELLA auxiliary circulatory pump catheters. We treat the most critically ill patients, including those in cardiopulmonary arrest due to cardiac causes and those with multi-organ problems requiring treatment from multiple medical departments.
We also focus on early social reintegration and prevention of recurrence after acute phase treatment. A team of doctors, nurses, nutritionists, pharmacists, physical therapists, and occupational therapists provide rehabilitation (link to rehabilitation explanation page), lifestyle guidance, and medication guidance. Even after discharge, in addition to outpatient support from doctors and nurses, we offer rehabilitation and nutritional guidance, supporting the team’s efforts to help patients return to their normal lives as quickly as possible and prevent recurrence of the same illness.
Treatment for Angina Pectoris (Chronic Coronary Syndrome)
We strive to provide optimal treatment for each patient with safety and peace of mind, considering the advantages and disadvantages of drug therapy, catheter treatment, and bypass treatment
In cases of angina where coronary blood flow gradually decreases, we administer medications to prevent blood clot formation (antiplatelet drugs), dilate coronary vessels (coronary vasodilators), and reduce cardiac stress (beta-blockers) to alleviate symptoms that cause discomfort in daily life.
Based on existing large-scale clinical research evidence, it has been proven that the above drug treatments are sufficiently effective for angina. In addition, there are ‘revascularization’ treatment methods that improve coronary blood flow reduced by atherosclerosis, such as balloon or stent treatment by catheter and bypass treatment by surgery. There is clear evidence that this revascularization improves symptoms and quality of life (QOL). For most patients, compared to drug treatment, the effects on extending lifespan (reducing mortality) or reducing future myocardial infarction occurrences are not clear. However, these effects can be expected in patients with severe ischemic heart disease, and our hospital performs revascularization treatment for patients who are considered to benefit from it after thorough consultation.
Percutaneous Coronary Intervention (Catheter Treatment)
World-class catheter treatment, minimized without unnecessary procedures
Catheter treatment for angina is a relatively low-burden procedure performed by inserting a catheter about 2mm in diameter through a blood vessel in the wrist or groin. Under local anesthesia, most treatments are performed by inserting a catheter from the wrist (some from the groin) to treat the coronary arteries using balloons or stents. The duration of treatment varies depending on individual circumstances, but typically takes about 2 hours if there are no special conditions. With wrist catheterization, patients can walk immediately after treatment and generally be discharged the day after treatment.
The principle of our center’s coronary artery treatment by catheter is to ‘provide necessary treatment to patients who need it, in the most appropriate way, safely and comfortably.’ The necessity of revascularization treatment such as catheterization for patients with ischemic heart disease varies for each individual. Many catheter treatments involve placing a lifelong mesh-like metal tube called a stent in the coronary artery. Since it’s not as simple as ‘inserting a stent because the vessel is narrow,’ our hospital thoroughly considers the necessity and proposes appropriate treatment for each patient. In the United States, unnecessary catheter treatments were once pointed out, leading to a review of appropriate indications for catheter treatment (Appropriate Use Criteria). As a result, it was reported that the number of inappropriate catheterizations in the US halved. This is also considered to be the case in our country, and we have entered an era where ‘quality of treatment rather than the number of procedures’ is questioned. Our hospital places emphasis on the quality of treatment rather than the number of procedures in our practice.
In catheter treatment, we strive to provide safe and long-lasting (requiring no retreatment) treatment using world-class treatment devices such as drug-eluting stents and balloons, based on image information from coronary CT and intravascular imaging (IVUS/OFDI) using ultrasound and optical coherence, as well as coronary blood flow information from FFR and FFRCT.
For those who want to know more about the process of cardiac catheterization and treatment at our hospital, please refer to here.

Coronary Artery Bypass Surgery
Maximum effect with minimum burden
Surgery = high burden. Cutting into the body. This is probably what most people imagine first. Indeed, that’s true. On the other hand, what are the advantages of this treatment? To put it simply, after coronary artery bypass surgery, the life risk from coronary artery disease is almost canceled. In other words, receiving this treatment increases the probability of living almost as long as someone without coronary artery disease. Our surgical team strives daily to provide this treatment with the minimum possible burden.
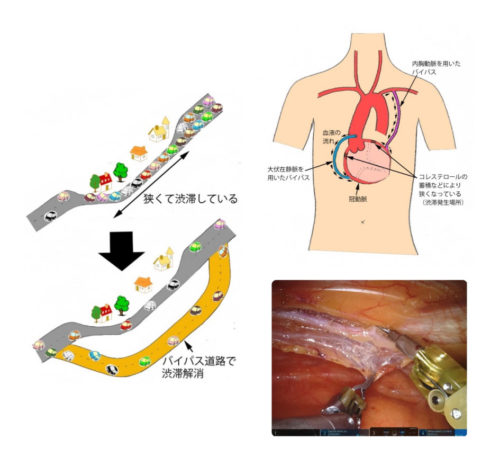
Coronary artery bypass treatment, as the name suggests, is a treatment that creates a bypass. It might be easier to understand if we compare it to a road bypass. When an old road frequently experiences congestion due to increased traffic, a bypass road is built to allow for smoother traffic flow. In this case, a new road is constructed from before the congestion starts to beyond where it ends. Coronary artery bypass treatment follows the same concept, using your own blood vessels to create a new blood flow by connecting before and after the narrow part.
The blood vessels used for bypass are the internal mammary artery, which flows vertically on the inside of the chest on both sides, and the great saphenous vein, which flows vertically on the inside of the leg. Sometimes, arteries from the hand or blood vessels from the stomach are also used. Among these, the internal mammary artery is known to be relatively long-lasting, so using this vessel is considered better. There is one internal mammary artery on each side, for a total of two. At our hospital, we use both internal mammary arteries in over 90% of cases to maximize effectiveness. Also, in over 90% of cases, we perform off-pump coronary artery bypass surgery without using a heart-lung machine.
Additionally, to make veins last longer and reduce the burden on the body, we generally harvest veins endoscopically while preserving the surrounding tissue.
As part of our efforts to minimize the burden on the body, we also perform robot-assisted internal mammary artery dissection. By making a small incision in the left chest for bypass, we aim for discharge within 5 days after surgery at the earliest.
Comprehensive Medical Care by the Heart Team
Treatment is decided not by a single doctor, but through discussions among doctors from various cardiac specialties, focusing not just on immediate treatment success but also on ‘wellness’ 10 years down the line
The Heart Team is a team composed of multiple doctors with various cardiac specialties and medical staff including nurses. When deciding on complex treatments, it is considered desirable for multiple medical professionals to consult in the Heart Team to determine the optimal treatment for each individual patient, rather than having a single doctor decide the treatment for a single patient. At our center, we hold daily Heart Team meetings to discuss and determine (propose) appropriate treatment methods for individual patients.
There are three coronary arteries in total, and ischemic heart disease with lesions in multiple vessels is often complex in treatment selection, making it a representative condition where treatment methods should be decided by the Heart Team. As mentioned above, the treatment methods proposed to patients with such conditions can be broadly divided into three categories: ①treatment with medication only, ②catheter treatment, and ③bypass surgery treatment. There are also combination treatments of catheter and bypass surgery. These patients do not uniformly have suitability for each treatment, and the degree of recommendation for each treatment differs depending on the state of coronary artery lesions, age, cardiac function, renal function, presence of comorbidities such as diabetes, etc. At our center, we discuss appropriate treatment choices for each patient in the Heart Team, considering not just immediate treatment success, but whether patients will be healthy 5 or 10 years after treatment, using objective data and taking into account individual patients’ values, family situations, and social backgrounds.
Safe and Short Hospital Stays
To help patients return to their normal lives as soon as possible, we achieve hospital stays of within 7 days for most acute myocardial infarction patients, 1 night 2 days for angina catheterization, and within 10 days for bypass treatment
The length of hospital stay is also an important consideration for patients. Our center strives to ensure that inpatients can return home as early as possible while maintaining safety.
In cases of acute myocardial infarction, although it varies depending on the severity, most patients can be discharged within 7 days if there are no problems during the hospital stay. The average hospital stay for acute myocardial infarction cases, including the most severe cases, is 7.1 days at our hospital (2021 in-hospital data) compared to the national average of 12.0 days (2021 DPC data survey) (link to ‘See St. Luke’s Quality’). While bodily safety is the top priority and stays may be longer than this period, we consider it important to safely return patients who suddenly had to be hospitalized to their homes in as short a period as possible. Also, for angina patients undergoing catheter treatment at our hospital, a 1 night 2 day stay is typical. For bypass surgery, compared to the national average of 21.8 days, our hospital’s average is 12.3 days (2021 in-hospital data).
