Physiological Function Tests
What is Physiological Function Testing
Electrocardiogram (ECG)
① Exercise Stress ECG
② Long-term ECG
-24-hour Holter ECG Monitor (24-hour ECG)
-Long-term ECG Recorder (Heart Note)
-Portable ECG Monitor
Cardiac Ultrasound Examination
① Stress Echocardiography
② Transesophageal Echocardiography
What is Physiological Function Testing
Physiological function testing is a general term for examinations that investigate the structure and function of the body through direct patient contact. The main tests include electrocardiogram (ECG), pulmonary function test, and electroencephalogram (EEG). In cardiovascular care, in addition to ECG, we perform exercise stress tests, cardiac ultrasound examinations, vascular ultrasound examinations, and blood pressure pulse wave tests.
Electrocardiogram (ECG)
The heart functions as a pump by repeatedly contracting and expanding as electrical stimuli are transmitted, sending blood throughout the body. An ECG examines the heart’s electrical activity to detect arrhythmias, cardiomyopathies, ischemic heart diseases, and other conditions. In addition to resting ECGs, our hospital also conducts exercise stress ECGs and long-term ECGs.
① Exercise Stress ECG
By recording ECG changes when the heart is under stress during exercise, we examine exercise-induced symptoms and ECG abnormalities. This is used for diagnosing ischemic heart disease and arrhythmias, and for determining treatment plans. At our hospital, we use treadmills, similar to room runners, and stationary bicycles called ergometers for exercise stress testing.
When necessary, we also perform cardiopulmonary exercise testing, which analyzes exhaled gases during exercise. This is an important test for determining the timing of surgery and assessing risks for pregnancy and childbirth. As a general hospital, we can usually schedule these tests relatively easily and provide results quickly without long waiting periods.

② Long-term ECG
By recording ECG during daily activities, we can detect arrhythmias or ischemic heart diseases (angina) that cause palpitations or chest pain, which might not be found in resting ECG tests. Our hospital offers 24-hour Holter ECG monitors, long-term ECG recorders (Heart Note), and portable ECG monitors.
-24-hour Holter ECG Monitor (24-hour ECG)
Five electrodes are attached to the chest, and a small monitoring device is worn while you go about your normal daily activities for 24 hours. Hospitalization is not required, but bathing (showering) is not allowed during the measurement. You will be asked to keep an activity log to correlate symptoms with ECG findings. This test reveals the timing and frequency of arrhythmias throughout the day. It’s excellent for detecting asymptomatic arrhythmias as it records during sleep. It can also be effective in diagnosing effort angina and variant angina. Some devices can also measure 24-hour blood pressure, which is useful for assessing home blood pressure, daily blood pressure variations, and treatment effectiveness.
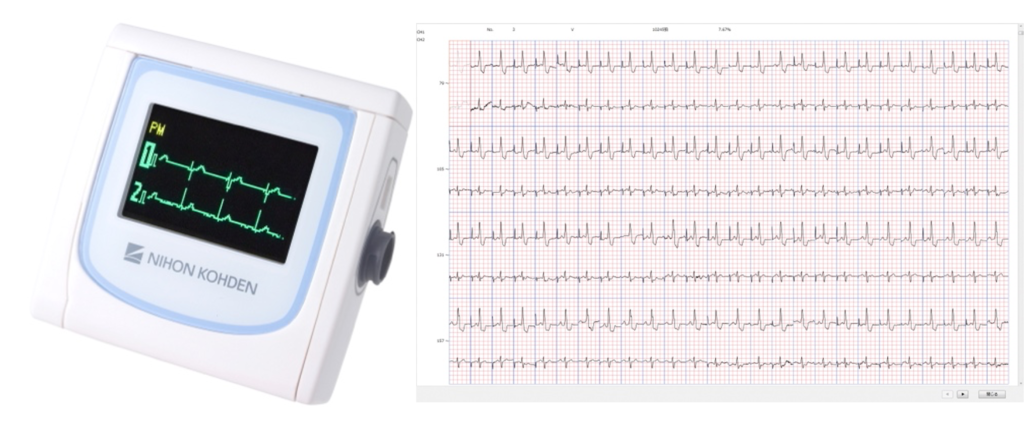
–Long-term ECG Recorder (Heart Note)
A lightweight, cordless ECG device about 10 cm in size with integrated electrodes is attached to the chest to record ECG. It can record for up to 7 days. Hospitalization is not required, and showering or partial bathing is possible during use. Even if arrhythmias are not detected in a 24-hour Holter ECG, recording for 7 days increases the likelihood of detection, contributing to early discovery and treatment. The long-term ECG recorder (Heart Note) is very convenient but not available at all hospitals. We often receive referrals from clinics for 7-day ECG recording.


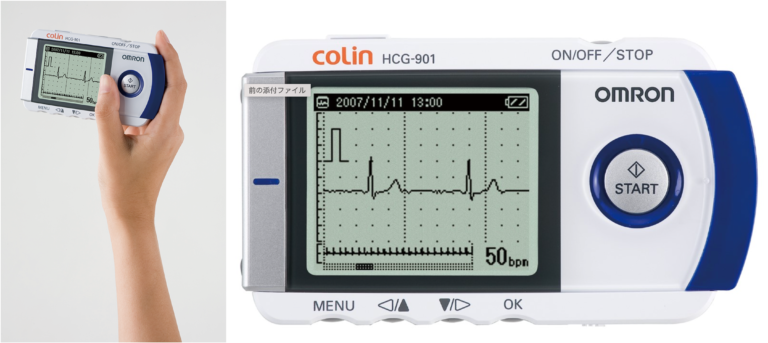
-Portable ECG Monitor
When symptoms such as palpitations or chest pain occur, you can place the portable ECG monitor on your abdomen to record the ECG on the spot. This helps determine if symptoms are due to arrhythmia or angina. While you need to carry the device, unlike Holter ECG or Heart Note, it doesn’t need to be attached to your body, so there’s no physical discomfort. Our hospital lends out the device for 7 days.
Cardiac Ultrasound Examination
This examination uses ultrasound to observe the size, movement, and blood flow of the heart. It excels at detecting structural abnormalities of the heart and is useful for diagnosing valvular diseases, cardiac hypertrophy, ischemic heart disease, cardiomyopathy, congenital heart disease, and heart failure, as well as determining severity, evaluating treatment effectiveness, and monitoring post-cardiac surgery progress. If necessary, stress echocardiography or transesophageal echocardiography may be added.
Using the latest echocardiography equipment, we can perform myocardial strain testing and 3D echocardiography. In the early stages of cancer treatment-related cardiomyopathy, cardiac amyloidosis, and other cardiomyopathies, relying solely on the conventional left ventricular ejection fraction (EF) may miss myocardial damage. Therefore, it’s important to diagnose early by detecting decreases in strain or its patterns. While very useful, not all hospital echo machines are equipped with this technology, and we often receive referrals from nearby cancer treatment facilities.

① Stress Echocardiography
This is a cardiac ultrasound examination performed while the heart is under stress from exercise or medication. Abnormalities that are not apparent at rest may become evident under stress. It is mainly used for diagnosing ischemic heart disease, hypertrophic cardiomyopathy, and valvular diseases, and for determining treatment strategies. It’s a particularly useful non-invasive diagnostic tool when suspecting cardiac valvular disease as a cause of exertional shortness of breath. At our hospital, we use treadmills and ergometers for exercise stress, but when exercise stress is difficult, we can also perform handgrip or pharmacological stress (dobutamine stress) echocardiography.
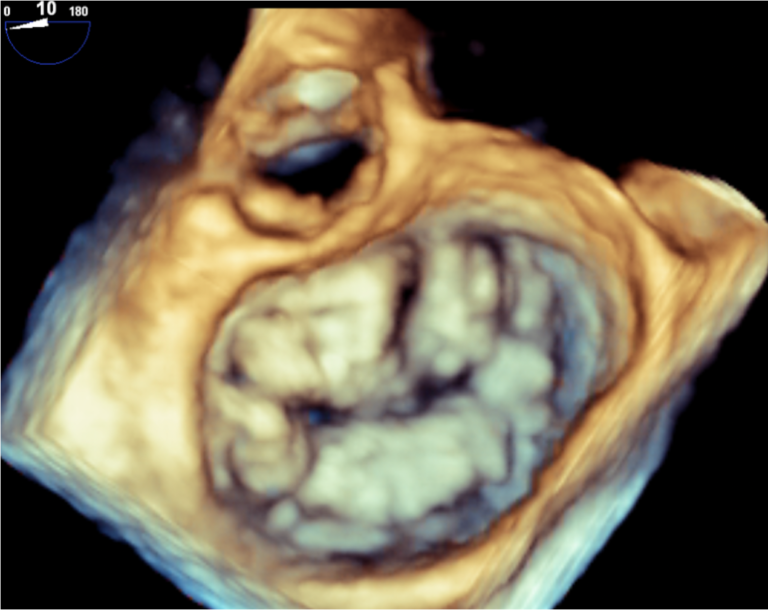
② Transesophageal Echocardiography
Similar to a gastroscopy, an ultrasound probe is inserted into the esophagus to observe the heart from the esophageal side. While the heart may be difficult to observe in standard ultrasound examinations due to bone and lung interference, transesophageal echocardiography provides clearer images. In most cases, sedatives are used to help patients sleep during the examination, minimizing discomfort. It is mainly used for diagnosing valvular diseases, infective endocarditis (heart infections), shunt diseases (conditions where small holes exist in the heart), and for detecting blood clots in the heart. Using the latest echocardiography equipment, we can obtain clear 3D images, allowing for more accurate understanding of cardiac structures, which aids in determining treatment plans and explaining conditions to patients. It’s particularly important to develop surgical strategies using realistic 3D cardiac images before heart surgery. Multiple ultrasound specialists attend the examination to ensure thorough assessment while minimizing patient burden and keeping the examination time relatively short.
Vascular Ultrasound Examination
This examination uses ultrasound on the blood vessels in the neck and limbs to examine the width of vessels, arterial stenosis or occlusion, presence of blood clots, and blood flow. It is used to diagnose atherosclerotic diseases in the neck and limb vessels and to detect blood clots in veins. Blood clots in the leg veins may be involved in causing leg swelling and pain. We also receive referrals from local clinics for patients who cannot undergo contrast-enhanced CT angiography due to allergies or for the evaluation of superficial varicose veins.
Blood Pressure Pulse Wave
This test simultaneously measures blood pressure in the upper limbs (arms) and lower limbs (ankles) to examine the degree of arteriosclerosis and vessel occlusion. It’s a test that reveals the so-called ‘vascular age’ and is useful for arteriosclerosis screening and lifestyle disease prevention guidance.
It is also used to diagnose peripheral arterial disease, which can cause numbness, pain, and cold sensation in the lower limbs during walking due to blocked blood vessels in the legs. As peripheral arterial disease progresses, it can lead to intractable leg wounds. In such cases, we may add an SPP (Skin Perfusion Pressure) test, which examines capillary blood flow, to determine the treatment plan.