Peripheral Artery Disease
Arteriosclerosis Obliterans of the Lower Extremities
Peripheral artery disease is a condition where arteries narrow due to atherosclerosis, resulting in poor blood flow mainly in blood vessels other than those of the heart (coronary arteries).
The majority of cases involve arteriosclerosis obliterans of the lower extremities (particularly when peripheral artery disease affects the legs), which can cause symptoms such as numbness and coldness in the feet, as well as skin peeling and ulcers.
What are the symptoms?
Generally, arteriosclerosis obliterans of the lower extremities is classified into four stages according to the Fontaine classification. It doesn’t necessarily progress from stage I to IV, and sometimes ulcers may form without prior notice.
Stage I: Asymptomatic (numbness, cold sensation)
Initially, there may be no symptoms, but caution is advised if you start feeling uneasy during long walks.
Stage II: Intermittent claudication
Pain occurs in the legs (especially in the calves) while walking, making it difficult to continue, but it subsides after resting for a while. This symptom is called “intermittent claudication.”
Stage III: Rest pain
As the condition progresses, pain may occur even at rest.
Stage IV: Ulcers/Gangrene
With further progression, blood flow to the feet may cease, leading to difficult-to-heal wounds (ulcers) on the feet, tissue death (necrosis) of the toes, and in some cases, the need for amputation of the lower limbs.

In cases of severe symptoms like Stage III and IV, with high risk of limb amputation due to tissue loss, nerve damage, or infection, the condition is called chronic limb-threatening ischemia (CLTI). This may require earlier consultation for treatment. (Previously, this was referred to as critical limb ischemia.)
Who is at risk?
It is known that smokers, people with diabetes, and those with kidney problems requiring dialysis are at higher risk of developing arteriosclerosis obliterans.
How is it diagnosed?
Medical interview, visual examination, and palpation
We confirm if there are any concerning symptoms as mentioned above through conversation. The progression of atherosclerosis can be somewhat determined by observing skin color and feeling the pulse in the feet.
Functional tests: ABI, etc.
ABI stands for Ankle Brachial pressure Index. It’s a test that measures blood pressure in the feet and arms simultaneously to compare the foot blood pressure to the arm blood pressure. If the ABI is extremely low (below 0.9) or extremely high (above 1.4), poor blood flow to the feet is suspected. Depending on the condition, we may also perform tests to measure toe pressure (TP) or skin perfusion pressure (SPP) to evaluate blood flow to the skin.
Imaging tests: Ultrasound, CT, MRI, angiography, etc.
To determine which blood vessels are affected, the extent of the condition, and its progression, we need to perform ultrasound, CT, or MRI scans. In cases where more accurate information is required, we may conduct an angiography, which involves injecting contrast medium into the leg’s blood vessels through a catheter and taking X-ray images.
How is it treated?
Treatment can be broadly divided into medical and surgical approaches. In cases of chronic limb-threatening ischemia (CLTI), we consult with various other departments such as infectious diseases, dermatology, and plastic surgery to develop a highly individualized treatment plan for each patient.
Medical treatment
Conservative treatment (drug therapy and exercise therapy)
We may use antiplatelet drugs (blood thinners), statins (cholesterol-lowering drugs) to prevent the progression of atherosclerosis, and vasodilators.
Additionally, exercise therapy is recommended, involving walking at an intensity that causes claudication, resting when pain becomes moderate, and repeating this process. It is recommended to do this for 30-60 minutes per session, three times a week for at least three months.
Catheter-based revascularization (EVT: endovascular therapy/endovascular treatment)
Similar to heart vessel treatments, we use catheters to widen narrowed blood vessels with balloons or place stents. However, the choice of stent or balloon treatment is determined by specialists based on the blood vessel’s condition and shape.
Surgical treatment
Thromboembolectomy
This method involves directly cutting into the artery with poor blood flow and removing the causative lesion. It is often performed for lesions in the groin (inguinal region) or behind the knee (popliteal region) where stent treatment (endovascular therapy) is not preferred.
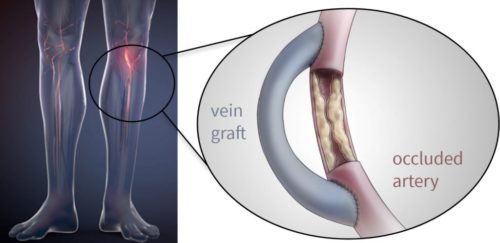
Bypass surgery
This method creates a detour (bypass) to replace the artery with poor blood flow. The bypass material can be the patient’s own vein or an artificial blood vessel.
At our hospital, we hold daily conferences between the cardiovascular medicine and cardiovascular surgery departments. The choice of treatment method needs to be determined comprehensively, considering the patient’s overall condition, the location and length of the lesion, and the state of the legs.
Please refer to this site created by Medical Note as well.
For those who want more specialized information, there is a guideline revised by the Japanese Circulation Society in 2022.
There are also many other sites created by various organizations, so we recommend using them comprehensively.
Japanese Society for Vascular Surgery: What is Peripheral Artery Disease?
Otsuka Pharmaceutical: What kind of disease is PAD?
Boston Scientific: Do you know about the disease called PAD?
NHK Health Channel: Peripheral Artery Disease (Arteriosclerosis Obliterans)
